COVID-19 Special Summer Edition
During these unprecedented times, it is our job to ensure our community has the most up-to-date, accurate information.
You may still have lots of questions about the novel coronavirus, and we’re here to answer them. Our earlier post Coronavirus and Your Heart gave an overview of what we knew about COVID-19 at the time.
What is COVID-19?
SARS-CoV-2, more popularly referred to as “COVID-19,” belongs to the family of viruses called the coronaviruses because of their crown-like appearance. The origin of the virus is largely debated; however, we know this virus is transmitted from person to person.
What Are the Common COVID-19 Symptoms? *
- Fever or chills
- Cough
- Shortness of breath or difficulty breathing
- Fatigue
- Muscle or body aches
- Headache
- New loss of taste or smell
- Sore throat
- Congestion or runny nose
- Nausea or vomiting
- Diarrhea
*An important note is that many individuals will not experience symptoms until 2-14 days after exposure. This is why it is so important to avoid crowds and non-essential outings.
If you have a fever or any kind of respiratory difficulty such as coughing or shortness of breath, call your doctor or a health care provider and explain your symptoms over the phone before going to the doctor’s office, urgent care facility, or emergency room. If you have a medical emergency such as severe shortness of breath, call 911, and tell them about your symptoms.
How Can I Prevent the Spread of COVID-19?
The best thing you can do to keep yourself and others safe in the fight against COVID-19 is to follow all the CDC Guidelines. “The most important precautions you can take are the same as for the regular flu: Wash your hands thoroughly and often, clean frequently touched surfaces, cover your mouth when you cough and sneeze, avoid traveling to areas with an outbreak, and stop touching your eyes, nose, and mouth. Stay home if you feel sick,” suggests Dr. Stephanie Coulter, MD, Director of the Center for Women’s Heart & Vascular Health and Texas Heart Institute Assistant Medical Director. There is no known cure or vaccine for COVID-19.
Where Can I Get Tested?
If you reside outside of Houston, we suggest checking your state’s Department of State Health Services webpage.
What is the Difference Between Viral Tests and Antibody Tests?
Viral Tests
These tests identify whether you currently have coronavirus. Consider this option if you are experiencing symptoms related to COVID-19.
Antibody Tests
These tests can identify whether you previously had COVID-19. After the onset of symptoms, these tests correctly identified only 70% of people who had COVID-19. ( How accurate are antibody tests? Learn More)
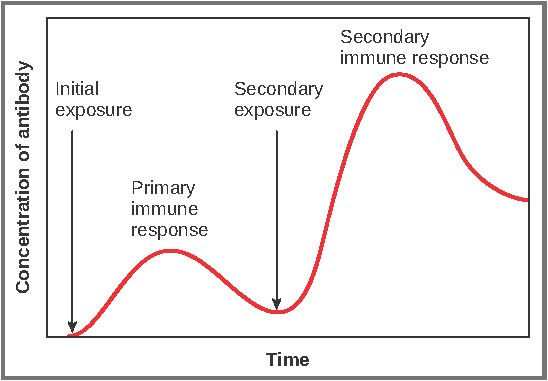
Source: OpenStax, Lumen Learning &. “Anatomy and Physiology II.” The Adaptive Immune Response: B-Lymphocytes and Antibodies | Anatomy and Physiology II, courses. lumenlearning.com/suny-ap2/chapter/the-adaptive-immune-response-b-lymphocytes-and-antibodies/.
How Do Antibodies Work?
Antibodies are part of the body’s immune response and protect us against infections caused by viruses and bacteria. Whenever you get exposed to a new infectious agent, your body makes antibodies to defend against a new disease but every time you get sick and overcome the illness, your body is flooded with antibodies that help combat the disease. These antibodies stay in your system and if you are exposed a second time, your body, using these antibodies, can fight off the infection with a strong, quick response.
Information to Keep in Mind About Testing
- Healthy individuals with only mild illness typically recover with no medical supervision or care.
- There is no cure, so testing positive only indicates that you should self isolate. If you require hospitalization, medical professionals can help treat the symptoms but cannot cure the disease.
- If you test positive and your symptoms worsen, call 911.
- Testing negative on a viral test indicates that you did not have COVID-19 at the time of testing. It does not mean you cannot get COVID-19 at a later time or that you are immune to coronavirus.
High-Risk Patients
According to the CDC, people who need to take extra precautions are those considered “high risk,” which includes people who are older than 65; those who have asthma, HIV, severe obesity, serious heart conditions, diabetes, or kidney or liver disease; and those who are immunocompromised. Smoking also increases the risk of death and complications due to COVID-19.
What does “Immunocompromised” Mean?
You may have heard the word “immunocompromised” when underlying conditions in vulnerable populations are mentioned. This means your immune system is unable to perform at its normal ability. These individuals are unable to build up these disease-fighting antibodies or sometimes even produce them at all, so when they get ill, they are unable to fight off the disease as well as healthy people can.
Does Pregnancy Increase Your Risk of COVID Infection?
From the current experience, it appears that pregnant women who become infected with COVID-19 are at an increased risk of requiring intensive care until admission and even intubation. It is not entirely clear why this occurs but is hypothesized to be due to a relatively immunocompromised immune system while pregnant. There also appears to be an increased risk of preterm delivery in women affected by COVID-19. The effects of COVID-19 infection during pregnancy on the fetus have yet to be formally described. The CDC recommends that pregnant women, in particular, must be diligent in practices the safe habits of social distancing, hand washing, and mask-wearing to protect themselves and their fetus
Current Statistics In-Hospital Death Among COVID-19 Patients.
-
- Coronary Artery Disease:10.2% vs. 5.2% among those without disease
- Heart Failure:15.3% vs. 5.6% among those without heart failure
- Cardiac Arrhythmia:11.5% vs. 5.6% among those without arrhythmia
- Current Smoking: 9.4% vs. 5.6% among former smokers or nonsmokers. (Read Smoking: It’s Not Just About the Lungs)
SOURCE: New England Journal of Medicine
You can view the full list of at-risk populations on the COVID-19 Information page.
How to Minimize the Spread?
To summarize, we’ll leave you with a quick recap of some of the things addressed here. When you can’t quarantine and have to be around other people in places like work, the grocery store, and other essential activities, social distancing (staying at least 6 feet from others) is strongly advised. Everywhere you go, practice frequent hand-washing with soap. The visual below explains how soap works and why it’s helpful in combating the virus. Resources for Kids & Families on Handwashing How Soap Works
What is the Difference Between Quarantining, Self-Isolating, and Social Distancing?
- Quarantine: This means that someone who may have been exposed to areas with a high number of COVID cases or to an actual COVID-19 positive case should stay away from others for at least 14 days to prevent the potential spread of the virus.
- Self-isolation: Similar to self-quarantine, self-isolation usually means that someone who is sick or has tested positive for the coronavirus eliminates all direct physical contact with others.
- Social distance: This practice involves staying at least 6 feet from other people. Six Feet = equals
- Two grocery carts end to end
- Two arms lengths
- Width of a sofa
- Width of a medium-sized car or sedan
SOURCE: CDC
What are the Ongoing Efforts to Defeat COVID-19?
- Wearing Masks
- Contact Tracing
- Research ( vaccines, best practices, new treatments & protocols, epidemiology…)
- Education, education, education
For more detailed talks from our cardiologists at Texas Heart Institute, visit our Cardiology in the Time of COVID-19 video library. Our episodes discuss Testing, Treatments & Vaccines, Digital Medicine, our take on the Status of the Pandemic, and Cardiovascular Medicine & COVID- Knowns and Unknowns much more!
Until Next Time!

Thank you to Dr. Karla Campos and Jackie Ferrufino for their contributions to this issue of Straight Talk.




