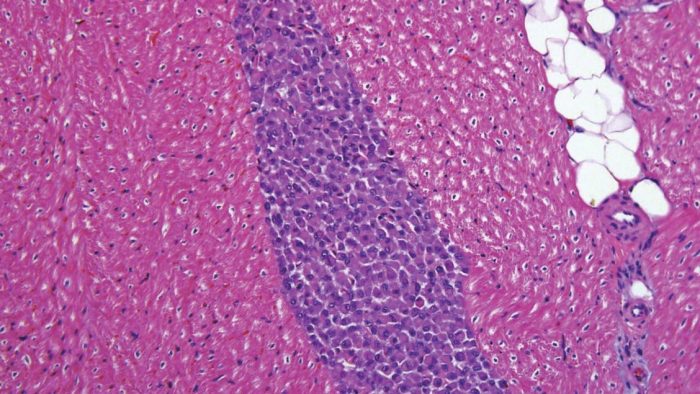
Through the department’s prestigious partnership with the Cardiovascular Cell Therapy Research Network (CCTRN) and industry sponsors, several clinical trials are currently underway. These clinical studies leverage previous discoveries and findings made by the department and represent a promising path to the first approved cell therapy to treat heart failure.
Stem Cell Center


Pioneers for the last two decades
Texas Heart Institute’s Stem Cell Center (SCC) seeks to leverage the regenerative properties of stem cells to help patients suffering from cardiovascular disease by improving treatment options and even reversing the effects of disease or damage to the heart. At the helm of this innovative department is the world-renowned physician-scientist Emerson Perin, MD, PhD, who has been a leader in cardiovascular stem cell research for more than 18 years.
Current Projects
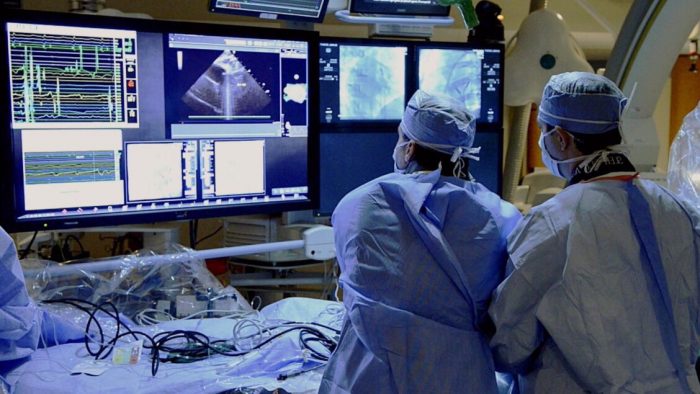
Learn more about our ongoing research projects and clinical trials that are designed to uncover groundbreaking insights that will bridge the basic science understanding of stem cell action with bedside treatment strategies for patients.
Stem Cell Center
With initiatives focused in basic and clinical research, the Stem Cell Center seeks to leverage the regenerative properties of stem cells to help patients suffering from cardiovascular disease by improving treatment options and even reversing the effects of disease or damage to the heart. The team also utilizes their discoveries to further stem cell therapies across all areas of medicine.

.svg)